Spinal Canal Stenosis
“Severe pain and numbness from spinal canal stenosis… don’t give up—consult us first.”

Are you experiencing any of these problems?
-
Suffering from chronic lower back pain
-
Numbness from the buttocks down to the legs
-
Relying on medication for pain and numbness
-
Using painkillers or nerve block injections to get by
-
Severe numbness that prevents you from walking for long periods
-
Pain when getting up in the morning
-
Attending massages repeatedly, but seeing no improvement
Your concerns
Leave it to Re:Light!
“The pain and numbness in both legs have gone, and I’m now able to sleep through the night.”
What Is Spinal Canal Stenosis?

Spinal canal stenosis is a condition in which the spinal canal—the passageway for nerves in the spine—narrows due to aging or other factors, compressing the nerves and causing pain or numbness. A characteristic symptom is ‘intermittent claudication,’ where numbness or pain in the legs worsens while walking and improves with rest. Symptoms also tend to ease when the lower back is flexed forward.
Common Age Groups and Related Conditions

Spinal canal stenosis is common in people over their 50s, and among those aged 65 and older, about one in ten are affected. It is also frequently seen alongside other conditions, such as lumbar spondylolisthesis or scoliosis.
Common Treatments Provided at Medical Facilities
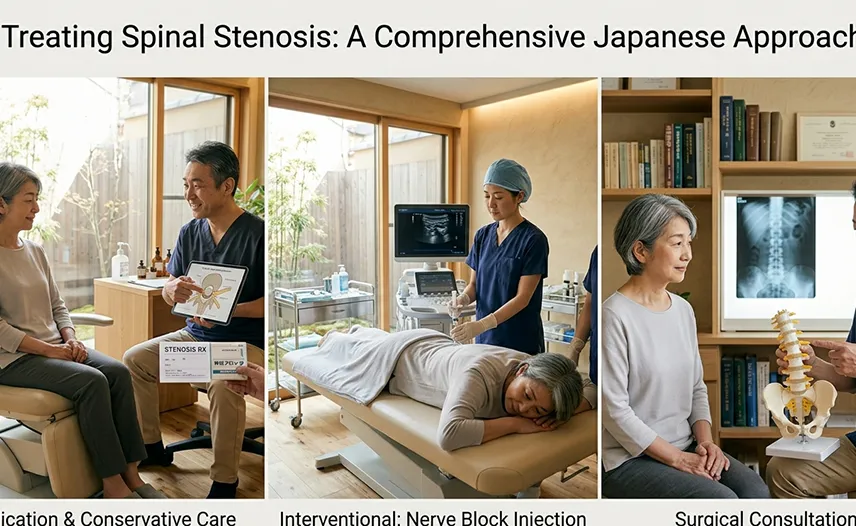
At medical facilities, treatments typically include medications, nerve block injections, and rehabilitation. However, if there is muscle weakness or urinary dysfunction, a surgical procedure called decompression may be required to widen the nerve passage.
Challenges of Surgical Treatment and Symptoms That Tend to Persist
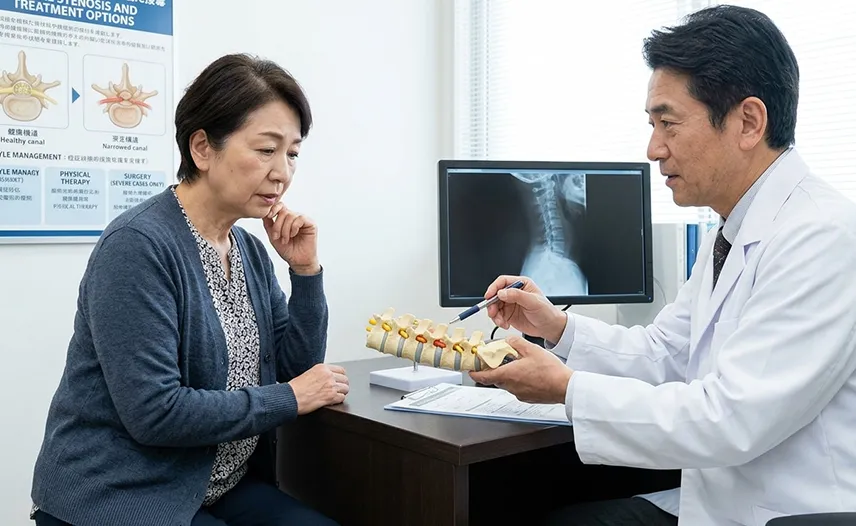
Surgery for spinal canal stenosis is very challenging, and doctors often recommend it only in the most severe cases. As a result, many people suffer from persistent symptoms for a long time without improvement.
Our Approach

At Re:Light, we begin by sharing information through careful listening and observing how the body is currently perceived, then explaining the overall direction of how sessions may proceed. If it seems appropriate to consult a medical institution, we may encourage considering that option.
During sessions, we do not focus only on areas of concern.Instead, we incorporate fascia‑based perspectives and pay attention to whole‑body connections, supporting awareness of movement and body usage.
Through this approach, we value ways of engaging with the body that make it easier to feel less strain during everyday activities.
